Lisa Maurer, MD, FACEP
Lisa Maurer, MD, FACEP
WACEP Past-President & Current Legislative Chair
“I love it here,” my patient at the Alternate Care Facility (ACF) said, and if I hadn’t been wearing a respirator, my jaw may have dropped. Since my EM group staffs the ACF, I knew the quality of care would be excellent. However, I didn’t expect the patients to feel so relaxed and comfortable in the middle of a state fair exposition center.
During my recent first shift working at the ACF, I saw patients who were happy to come from overwhelmed hospitals to receive expert care, provided by warmly attentive staff, in a surprisingly relaxing environment. If open inpatient beds are disappearing and ED holds are growing at your shop, I hope the details of my experience working at the ACF help you to convey the benefits of transfer to the ACF to your next patient with COVID.
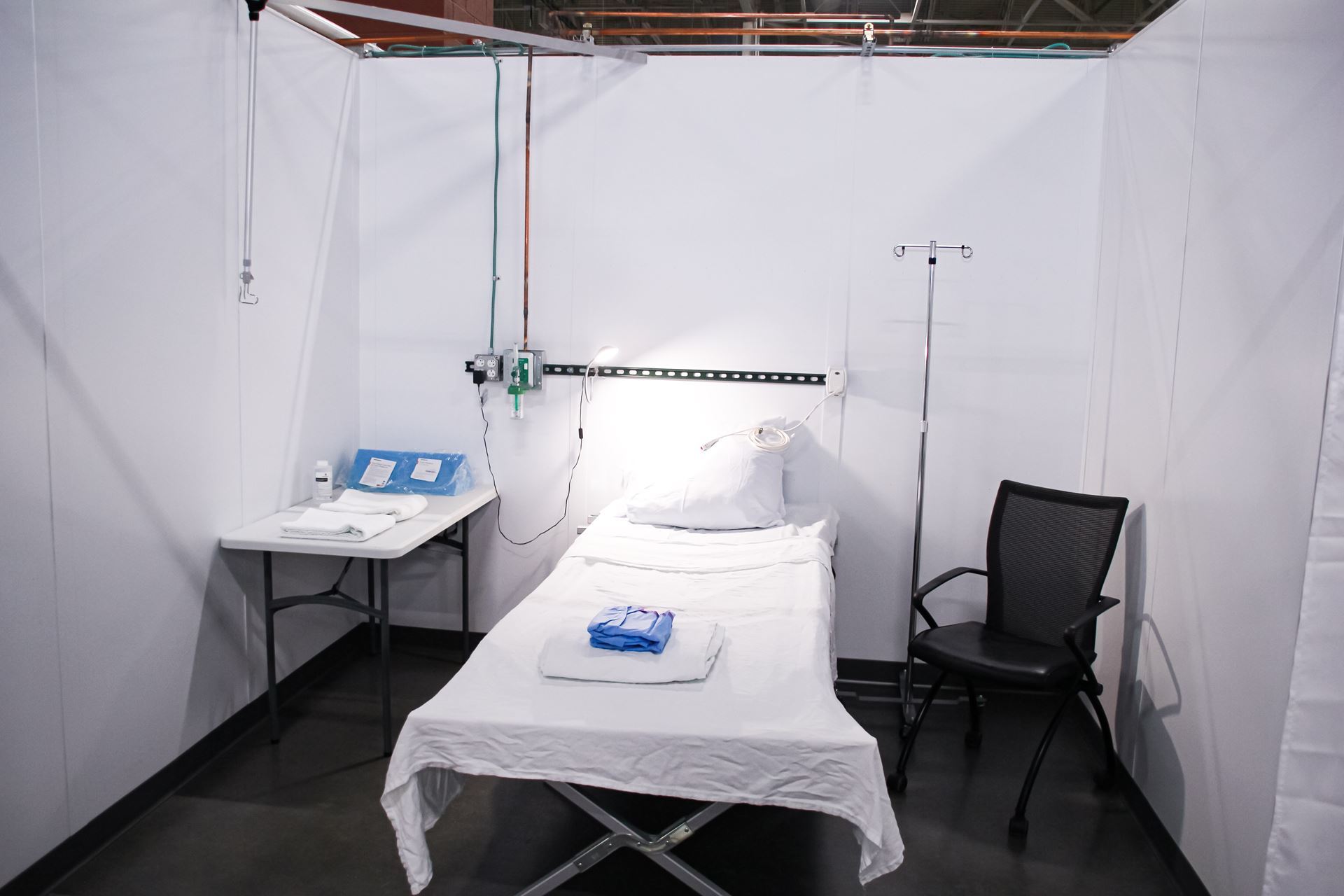
 After being propped up by the U.S. Army Corps of Engineers in the Spring, the ACF was activated on October 16th to serve as an overflow facility for Wisconsin. Check out this 15-second time lapse video showing the process of turning an Expo Center into a facility with the capacity to care for hundreds of patients. “Cubicle” type rooms are surprisingly quiet and have hospital beds. It’s not uncommon to see a patient’s room featuring a blanket or keepsake from home. Catered food is available three times daily, and on game day, the patients might be found in the common area by the big screen. There are pods of bathrooms and showers for those who feel up to it. Patients told me that they were getting more rest there than they were ever able to get in the hospital or even at home.
After being propped up by the U.S. Army Corps of Engineers in the Spring, the ACF was activated on October 16th to serve as an overflow facility for Wisconsin. Check out this 15-second time lapse video showing the process of turning an Expo Center into a facility with the capacity to care for hundreds of patients. “Cubicle” type rooms are surprisingly quiet and have hospital beds. It’s not uncommon to see a patient’s room featuring a blanket or keepsake from home. Catered food is available three times daily, and on game day, the patients might be found in the common area by the big screen. There are pods of bathrooms and showers for those who feel up to it. Patients told me that they were getting more rest there than they were ever able to get in the hospital or even at home.
 From a medical standpoint, almost 300 of the cubicles have in-line oxygen with capabilities for nasal cannula, high flow, or opti-flow up to 50L at 50% FiO2. They can receive IV fluids and medications, including remdesivir. As of the time of this article’s publication, there were 18 patients at the ACF with 6:1 nursing ratio and two providers. The onsite pharmacist is top notch, and many of the nurses and RTs are “travelers” who are more than comfortable caring for patients with COVID given their vast experience. In the case where a patient needs respiratory support or other medical care than surpasses what’s readily available, the onsite EMS unit transfers them to a nearby hospital at the discretion of the onsite emergency physician.
From a medical standpoint, almost 300 of the cubicles have in-line oxygen with capabilities for nasal cannula, high flow, or opti-flow up to 50L at 50% FiO2. They can receive IV fluids and medications, including remdesivir. As of the time of this article’s publication, there were 18 patients at the ACF with 6:1 nursing ratio and two providers. The onsite pharmacist is top notch, and many of the nurses and RTs are “travelers” who are more than comfortable caring for patients with COVID given their vast experience. In the case where a patient needs respiratory support or other medical care than surpasses what’s readily available, the onsite EMS unit transfers them to a nearby hospital at the discretion of the onsite emergency physician.
In response to feedback from around the state, the intake form has once again been revised and simplified. If you have a patient in your ED that meets the eligibility criteria as per the Reference Guide, fill out pages 4-5 of the guide and email to the address listed. The information will be reviewed by the CMO or designee, who is another fellow emergency physician. They review patients for transfer daily from 9a-5p, and patients may now arrive until 6:30p, updated from a previous 5p arrival deadline.
Everyone involved wishes we didn’t need an ACF. However, if you’re like me, I’m so grateful to have it as an option, especially now that I know it has proven to be a good experience for patients. I would expect nothing less than the EM physicians of Wisconsin to lead the effort in managing patient flow around our state as we continue to fight this pandemic.
 Editor’s Note: this article was written for informational purposes only and does not constitute any endorsement of care. The author, the author’s independent group practice/employer, and Wisconsin ACEP do not benefit in any manner from the transfer of patients or their care at the Alternate Care Facility in Milwaukee, WI.
Editor’s Note: this article was written for informational purposes only and does not constitute any endorsement of care. The author, the author’s independent group practice/employer, and Wisconsin ACEP do not benefit in any manner from the transfer of patients or their care at the Alternate Care Facility in Milwaukee, WI.